
The following proposal, “Clarifying and Strengthening the Party’s Program,” was made by the West Philadelphia Club and adopted for discussion by the National Board, CPUSA.
Party Program — Current position on healthcare
Healthcare is central to the life of every individual. Yet, the current Party Program does not contain a detailed analysis of the state of healthcare in the US. The section titled Health Care Struggles notes “U.S. capitalism’s aversion to ensuring health care as a human right” and expands on the challenges that working people face, particularly before passage of the Affordable Care Act (ACA). The Program also notes the growing support for more comprehensive healthcare reform, especially during the COVID pandemic.1
Moreover, the Program notes,
Removing the profit from the Wall Street–controlled health industry can fully fund a system that puts health before profit. Communists support comprehensive and free guaranteed access to quality care whenever needed, and the more robust funding of preventative programs. Until socialized medicine is achieved, the CPUSA advocates protecting and expanding the Affordable Care Act and implementing Medicare for All.
The demand for comprehensive and high-quality medical care, which by definition includes its concurrent access, is important and must be made known at every possible opportunity. Yet, the call to protect and expand the ACA while advocating for Medicare for All misses a profound opportunity to stake a stronger and more coherent position. Additionally, neither the ACA nor Medicare for All as currently proposed fundamentally addresses any of the other issues justly highlighted by the Party Program (e.g., for-profit health insurance and “supplemental” health services, pharmaceutical interests and drug pricing, medical education and training, the intimate connection between health and a community’s built environment) that would continue to plague the healthcare system even after adoption of a single-payer insurance system. Within this section the Party Program also outlines a specific policy proposal regarding medical education, noting,
A comprehensive health care system would mean that all health workers in hospitals and community clinics must reflect the populations they are serving — we support the aggressive application of affirmative action programs for equal access to medical, nursing, and other professional training and education programs.
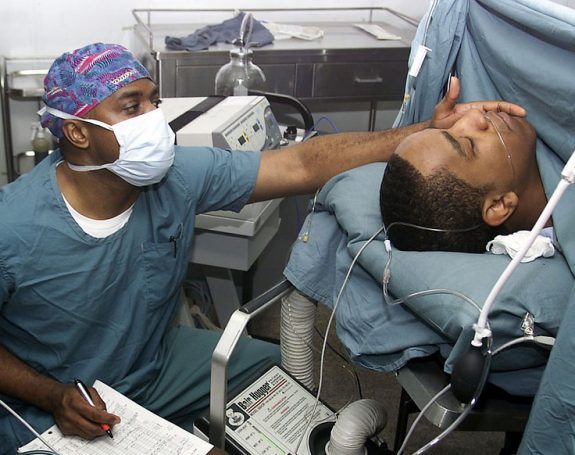 The lack of diversity and minority representation in medicine is a historic and ongoing problem that certainly must be addressed aggressively. Consider that between 1997 and 2017 there was a 63% increase in people from underrepresented groups in the US population (defined as American Indians/Alaska Natives, Blacks, Hispanics/Latinos) with a simultaneous 20% decrease in medical school matriculants from underrepresented groups per 100,000 of the population.2 In addition to racial/ethnic disparities in admission, there is also a clear class disparity as well. Between 1987 and 2005 the proportion of medical school applicants from the lowest quintile of US households did not exceeded 5.5%. In contrast, half came from the richest quintile.3 However, in addressing this problem the Communist Party must note that this will be done without compromising the quality of medical education and training. Given the nature of medicine and the responsibilities of healthcare workers, instituting quotas for admission to current undergraduate and graduate medical programs is, perhaps, less likely to draw general public support than removing the substantial barriers that exist to entry to professional training and education programs, including prohibitive exam fees, program application fees, and outlandish educational debt.4 Properly funding both primary and secondary education is a necessary concomitant change that would help bring more representation to medical training and education. A total restructuring of medical education (including nursing and other allied health professions) is also worth exploring and is discussed in a later section.
The lack of diversity and minority representation in medicine is a historic and ongoing problem that certainly must be addressed aggressively. Consider that between 1997 and 2017 there was a 63% increase in people from underrepresented groups in the US population (defined as American Indians/Alaska Natives, Blacks, Hispanics/Latinos) with a simultaneous 20% decrease in medical school matriculants from underrepresented groups per 100,000 of the population.2 In addition to racial/ethnic disparities in admission, there is also a clear class disparity as well. Between 1987 and 2005 the proportion of medical school applicants from the lowest quintile of US households did not exceeded 5.5%. In contrast, half came from the richest quintile.3 However, in addressing this problem the Communist Party must note that this will be done without compromising the quality of medical education and training. Given the nature of medicine and the responsibilities of healthcare workers, instituting quotas for admission to current undergraduate and graduate medical programs is, perhaps, less likely to draw general public support than removing the substantial barriers that exist to entry to professional training and education programs, including prohibitive exam fees, program application fees, and outlandish educational debt.4 Properly funding both primary and secondary education is a necessary concomitant change that would help bring more representation to medical training and education. A total restructuring of medical education (including nursing and other allied health professions) is also worth exploring and is discussed in a later section.
With the country still in the grips of the COVID pandemic, the political tides seem to be shifting in favor of more substantive changes to healthcare, but without taking the initiative the Communist Party could miss an opportunity to create a stronger and more comprehensive official position and to lead the advance for reforms that are truly transformative and equitable.
Single-payer healthcare (M4A) — advantages and disadvantages
The struggle for healthcare reform in the US, particularly with regard to health insurance, is not new. Contemporary efforts to expand health insurance in the US can be traced back to the ’70s, when healthcare activists argued over which model of healthcare insurance to advance: Canada’s National Health Insurance (NHI) or England’s National Health Service (NHS).5 Both models provide universal insurance coverage, but the former does not directly employ physicians, nurses, and other healthcare workers whereas the latter has a largely publicly owned and operated system. Other major differences include limitations to private, for-profit insurance and the ability for the wealthy to access care outside public wait lists. A national group was eventually formed called Physicians for a National Health Program (PNHP) that advocated for a Canadian-style reform, which largely remains in the same form today.6

Recent legislative proposals in Congress (HR676, HR1384, and S1129) all take as their foundation a Canadian-style reform. The promises of these single-payer “Improved and Expanded Medicare for All” proposals include elimination of most (but not all) private insurance, reduction in the size and scope of administrative bureaucracy and associated cost, and lower pharmaceutical drug prices through governmental collective bargaining. Despite these very real, potential advantages that would greatly benefit the mass of working people, there are significant limitations to current Medicare For All proposals. These include explicit continuation of for-profit health insurance (albeit supplementary), continuation of private ownership of hospitals and health systems, continuation of for-profit pharmaceutical companies, and continuation of current funding mechanisms and incentives for medical research and publication, drug discovery/trials, as well as medical education and training. These limitations directly impact the infrastructure and delivery of healthcare and must be addressed openly and honestly. Together with other long-standing trends that continue to shape how medicine is practiced and healthcare is delivered, not addressing the numerous remaining issues is likely, at best, to bring about a “two-tiered” system in the future. Evidence of this evolution can be seen in the healthcare systems of other major industrialized countries, with all of the disadvantages that come with it.7 More importantly, Medicare for All proposals do nothing to address the deepening proletarianization of physicians, nurses, pharmacists, medical assistants, technicians, etc.
The Party Program is particularly weak in this regard. To begin, the Party can decide if at this moment it principally values a defense of the ACA or a push to advance Medicare for All, given that these are mutually exclusive positions. The ACA is fundamentally a deepening of the private, for-profit insurance market and carries an implicit defense of the profit motive within healthcare. That there are specific, individual, and positive clauses/reforms within the law does not equate to a defense of the law as such. The COVID pandemic has demonstrated the insufficiency and insanity of reliance on employer-sponsored health insurance. Moreover, even prior to the COVID pandemic, health insurance premiums of ACA marketplace plans are increasingly unaffordable for working people.8 A shift to advancing Medicare for All, despite its limitations, is an improvement to a continued, explicit defense of the ACA. As Marxist-Leninists, the Communist Party is capable of explaining the material conditions within which healthcare workers labor and formulating solutions that provide redress from the alienation that healthcare workers experience. Possible solutions addressing this issue are absent from the Party Program.
Additionally, discussing the limitations of Medicare for All openly and honestly gives the Party intellectual credibility among healthcare workers especially, who understand that these reforms are largely positive for “consumers” but are either neutral or detrimental for them.
Unresolved challenges — medical education
As discussed previously, there are large disparities within medical education that often continue to go unmentioned in the larger discussion of healthcare reform. Representation within medicine must be addressed aggressively, but so too must other connected issues that are rarely discussed. Educational debt is a major obstacle and disincentive for those who wish to train and work in healthcare. For example, the median educational debt for medical students in 2019 was $200,000, the median student loan debt for graduate nursing students in 2017 was between $40,000 and $54,999 in 2017, and the median educational debt for pharmacy students in 2018 was $160,000.9-11 This debt is in addition to any accumulated undergraduate educational debt.
Healthcare reform proposals sometimes include cuts to physician salaries, typically including unflattering portrayals of physicians, but these proposals do not simultaneously address the enormous burden of debt. Moreover, high educational debt coupled with the difference in salary between medical specialties provides some discouragement for medical students to pursue careers in primary care or family medicine, as these specialities have lower average pay. Additionally, the US healthcare system, and the medical schools and residency programs which operate within it, excel at undervaluing primary and preventative care, despite the lip service paid. There is a massive opportunity, therefore, for the Communist Party to demand as part of its larger list of reforms to the healthcare system that the costs of attendance for healthcare professional programs be covered entirely by the public. The salaries of resident/fellow physicians are already paid for by the government, and the argument can be made that the public funding of healthcare workers’ education is a reflection of their being a public good.
 Removing the financial burden of medical education, together with equalization of pay between medical specialities, is likely to help increase the number of physicians in primary care. Of course, these reforms should be considered within the context of increasing the total number of physicians and nurses educated and trained, and providing incentives for physicians to practice in rural and underserved communities. There are sufficient medical colleges in the US to achieve this goal, although the establishment of any new, properly accredited programs can be geographically targeted to better promote the education and local retention of underrepresented minorities.
Removing the financial burden of medical education, together with equalization of pay between medical specialities, is likely to help increase the number of physicians in primary care. Of course, these reforms should be considered within the context of increasing the total number of physicians and nurses educated and trained, and providing incentives for physicians to practice in rural and underserved communities. There are sufficient medical colleges in the US to achieve this goal, although the establishment of any new, properly accredited programs can be geographically targeted to better promote the education and local retention of underrepresented minorities.
Additionally, reforming the basic structure and funding of American medical education can be considered. Medical school in the US is 4 years (MD or DO), whereas, for example, medical education in France is a minimum of 8 years, between 9 and 11 years in the UK, generally 8 years in China, and 7–9 years in Australia. Discrepancies are often due to variable length of training programs. It is important to note that most countries begin medical education after high school rather than college/university as here in the US, saving students both time and money. The principle end goal of most international medical programs is the education and training of licensed and competent general practitioners (i.e., primary care/family medicine physicians), with additional training needed for specialization. Here in the US completion of medical school does not qualify an individual to practice medicine, so our education is structured around specific residencies (typically an additional 3–7 years) and fellowships (typically 1–3 years), which provide the actual training to practice medicine competently and independently. The structural difference in medical education here in the US together with the astronomical debt and pay discrepancy help explain the relative abundance of specialists in the US compared to other nations, where the vast majority of physicians are general practitioners. The prestige of medicine is also ripe for capture by opportunists, as evidenced by the proliferation of joint MD/MBA programs and the stream of medical graduates who leverage their degree to join corporate leadership or to start venture capital projects without ever being clinicians. Many long-standing and negative trends in medicine can be directly tied to the business-minded bureaucrats medical schools graduate.
Medical education is further fractioned in the US between allopathic (MD) and osteopathic (DO) schools. Contemporary graduates of either MD or DO programs are equivalent and equally qualified to practice medicine, the difference tied to the history of osteopathic medicine in the US, a pseudoscientific practice, and its continued use as a convenient and strategic marketing tool to attract applicants.12,13 This equivalency is underlined by the fact that residency programs previously open only to graduates of one school or another are now merged. The division between allopathic and osteopathic is antiquated, and reforms to medical education should strongly consider MD/DO merger into a uniform standard doctor of medicine (MD) degree.
Unresolved challenges — medical training and working conditions
Intimately connected to the unresolved challenges of medical education are those of the training of medical professionals and their working conditions. Medicare is responsible for covering a large part of the costs of residency positions that are accredited through the Accreditation Counsel on Graduate Medical Education (ACGME). The average first post-MD year stipend in 2019 was $57,000, which is meager considering their labor (roughly $14/hour, assuming 80-hour work week) and the revenue their labor produces, and this is in the context of a 2017 ACGME requirement change limiting work hours to 80 hours per week (vs. the “good old days” prior to 2003 when there were no limits).14,15 Unfortunately, residents continue to routinely surpass ACGME work hour requirements and then are made to fabricate work hours to match limits set by accrediting bodies due to fear of reprisal by their respective institutions. Resident physicians also work without protections afforded by unionization, as opposed to nurses. For example, during the COVID pandemic nurses were able to negotiate hazard pay for staffing COVID wards, but no such benefit was provided to resident physicians. In understanding this it is much easier to understand the epidemic of physician burnout and suicide, which have only worsened over time. An estimated 400 physicians commit suicide annually, leaving about 1 million patients without a physician.16,17 This is especially true during the COVID pandemic, when institutions (public and private) utterly failed in their responsibilities, with staggering rates of emotional and psychological trauma reported by all healthcare workers. Bourgeois academicians and liberal apologists wander aimlessly in their explanations, but for Marxist-Leninists the core issues are clear: the deep and accelerating trend of physician proletarianization, the intrinsic capitalist drive to maximize productivity and profit, and the gradual loss of autonomy are some of the principal reasons for the rise of burnout in medicine. Healthcare workers are increasingly alienated from their labor, and the result has a direct, negative effect on healthcare.18

No political party explicitly forwards demands to challenge institutional structures that perpetuate this injustice. Instead, it is much easier for individuals, hospitals, cities, states, and the federal government to cheer for “our healthcare heroes” and for Starbucks to provide a week of free coffee. Physicians, nurses, and other healthcare workers are not fooled: these are vacuous and performative gestures that amount to nothing more than pornography. There remains a real hunger among healthcare workers for someone to speak to their immiseration and to directly address their training and working conditions. The Communist Party can stake out a leading position on this issue and leverage its Marxist analysis to outline a path ahead that considers the social relations between physicians, nurses, pharmacists, technicians, etc., as well as together with patients in a transformative and equitable healthcare system.
Unresolved challenges — proliferation of non-physician providers
As discussion and popular debate surrounding Medicare for All has increased in recent years, so too has a general understanding that the US healthcare system is motivated by the same drive for profit as any other industry within a capitalist economy. Even legally designated non-profit institutions are not immune, and staff meetings regarding “efficiency, productivity, and cost-containment” are ubiquitous. It should come as no surprise, then, that medicine has overseen the proliferation of various non-physician professions since the ’60s, originally conceptualized as a convenient way to slow the growth of healthcare costs. Chief among these professions are the nurse practitioner (NP) and physician assistant (PA), which physicians created with the idea of cooperative team management of care and with physicians providing careful supervision. Early studies in the ’70s showed this model of team-based care to be effective at providing high-quality and cost-effective care. However, this model began to shift when NPs, and then later PAs and other non-physicians, sought to expand their role and practice rights.
Today, the American Association of Nurse Practitioners (AANP) lobbies heavily for full practice authority (FPA), which means that NPs would effectively practice medicine without the requirement of being supervised by a physician and without having completed medical education and training. The AANP notes that FPA is
the authorization of nurse practitioners to evaluate patients, diagnose, order and interpret diagnostic tests, and initiate and manage treatments—including prescribe medications—under the exclusive licensure authority of the state board of nursing.19
The crux of the argument made by NPs, and equally with PAs and other non-physicians, is that the care they provide is equivalent or superior to physicians’ and at a lower cost. However, as detailed by Drs. Niran Al-Agba and Rebekah Bernard in their book Patients at Risk, “there are no credible, well-designed scientific studies that support the safety and efficacy of non-physicians practicing without physician supervision.” Moreover,
While medical literature headlines and abstracts may imply that the non-physician practitioners being studied were providing care “independently,” the fine print reveals otherwise. A detailed reading of each article makes it clear that in every single study, physicians were available for consultation and supervision when non-physician practitioners ran into trouble. Proponents of independent non-physician practice are making a dangerous assumption: that if a non-physician can practice safely with physician supervision, as studies seem to indicate, then they should be able to practice equally as safely without physician involvement.20
 Additionally, NPs and PAs, relative to physicians, are more likely to order additional unnecessary diagnostic and imaging tests, prescribe antibiotics in the outpatient setting (potentially worsening the growing threat of multi-drug resistant microbes), make lower-quality referrals (complicating care and increasing costs), and overprescribe opioids (specifically compared to NPs/PAs in prescription-restricted states).21–24 As part of their lobbying efforts, NPs and PAs also claim that they expand access to primary care in rural and poorer communities, though again the evidence does not support this claim.25 Although there is a need for increased access to primary care for these communities, there is significant debate over whether the deficit is largely artificial, a reflection of maldistribution rather than too few physicians. This argument is supported by the fact that, like many other professions, physicians and NPs and PAs tend not to accumulate in poorer regions of the country. Highlighting these differences is not “punching down” or a blind exercise of power and control by physicians. These differences are highlighted to reflect the significant discrepancy in education and training between physicians and non-physicians. 26,27 Consider, for example, an experiment that the National Board of Medical Examiners (NBME) conducted from 2008 to 2014 where NPs seeking a doctoral degree were given the opportunity to take a less comprehensive version of the USMLE Step 3, an exam that resident physicians must pass before becoming licensed to practice medicine independently as attending physicians. Typical pass rates for Step 3 for US graduates of allopathic (MD) medical schools and osteopathic (DO) medical schools is around 97% and 94% respectively. The pass rate on the simplified Step 3 for NP doctoral students ranged from 33% to 70%, averaging around 50% over the five examinations conducted. The examination was discontinued in 2014 due to “limited utilization.”28 There is even opposition to the push for FPA by rank-and-file NPs and PAs, though they are explicitly told to remain silent by leadership.29 Still, the march to independent practice continues unabated, with legislators easily swayed by misleading information from lobbying groups or by powerful healthcare corporate interests whose bottom line is served by an expanding workforce of NPs and PAs.
Additionally, NPs and PAs, relative to physicians, are more likely to order additional unnecessary diagnostic and imaging tests, prescribe antibiotics in the outpatient setting (potentially worsening the growing threat of multi-drug resistant microbes), make lower-quality referrals (complicating care and increasing costs), and overprescribe opioids (specifically compared to NPs/PAs in prescription-restricted states).21–24 As part of their lobbying efforts, NPs and PAs also claim that they expand access to primary care in rural and poorer communities, though again the evidence does not support this claim.25 Although there is a need for increased access to primary care for these communities, there is significant debate over whether the deficit is largely artificial, a reflection of maldistribution rather than too few physicians. This argument is supported by the fact that, like many other professions, physicians and NPs and PAs tend not to accumulate in poorer regions of the country. Highlighting these differences is not “punching down” or a blind exercise of power and control by physicians. These differences are highlighted to reflect the significant discrepancy in education and training between physicians and non-physicians. 26,27 Consider, for example, an experiment that the National Board of Medical Examiners (NBME) conducted from 2008 to 2014 where NPs seeking a doctoral degree were given the opportunity to take a less comprehensive version of the USMLE Step 3, an exam that resident physicians must pass before becoming licensed to practice medicine independently as attending physicians. Typical pass rates for Step 3 for US graduates of allopathic (MD) medical schools and osteopathic (DO) medical schools is around 97% and 94% respectively. The pass rate on the simplified Step 3 for NP doctoral students ranged from 33% to 70%, averaging around 50% over the five examinations conducted. The examination was discontinued in 2014 due to “limited utilization.”28 There is even opposition to the push for FPA by rank-and-file NPs and PAs, though they are explicitly told to remain silent by leadership.29 Still, the march to independent practice continues unabated, with legislators easily swayed by misleading information from lobbying groups or by powerful healthcare corporate interests whose bottom line is served by an expanding workforce of NPs and PAs.
The political economy of capitalist healthcare demands that hospital, insurance, and government administrators and bureaucrats focus on cutting costs and maximizing revenue. The proliferation of non-physician providers has transformed into a vehicle to realize even greater profit for corporations and cost savings in public institutions like the Veterans Health Administration, but increasingly at the cost of patient care. Unfortunately, this issue is largely unknown to the public. Non-physicians are valued members of the healthcare team, but they are not interchangeable with physicians.
The Communist Party can include in its demands that the right to high-quality healthcare means the care is physician led. The demand could be summarized as, “Team-based, physician-led, and patient-centered healthcare is a right of every American.” Instead of prioritizing costs and revenue, the Communist Party can firmly establish itself on the side of patients and draw legitimacy in clearly defining what “high-quality healthcare” would actually mean in a transformed and more equitable healthcare system.
Unresolved challenges — pharmaceutical companies
Concomitant with the public correctly identifying the shear greed and capriciousness of insurance companies throughout the ongoing debate on Medicare for All is the identification of pharmaceutical companies interests’ being diametrically opposed to those of the public. Occasional popular uproars over drug prices (e.g., insulin, EpiPens, chemotherapeutics) have motivated reformers to also consider the power of pharmaceutical companies when devising and organizing for reforms to healthcare. Yet, particular myths endure, which we as communists would be wise to challenge directly. As noted by Joel Lexchin in the book Health Care under the Knife,
The myth is that its profits come from producing and selling the many therapeutic advances that industry research has generated, but the reality is far different. In the first place, after tax deductions only about 1.3 percent of the money that the industry spends actually goes to basic science research, the type of research that leads to new medications. Second, most of the new medicines that come from the pharmaceutical corporations offer little to nothing in new therapeutic options. For the decade 2005 to 2014, among 1,032 new drugs and new uses for old drugs introduced into the French market, for example, only sixty-six offered a significant advantage whereas more than half were rated as “nothing new,” and 177 were judged “unacceptable” because they came with serious safety issues and no benefits.
The industry also justifies its high levels of profits with the claim that drug development is inherently risky. To this end, the pharmaceutical corporations maintain that only one in every 10,000 molecules actually results in a new drug. Though this may be true, most of the molecules that fall by the wayside do so in the very early stages of development when costs are minimal. The $2.6 billion figure that is now cited as the cost to bring a new drug to market comes from data that is confidential, and the calculations are based on a set of assumptions that have been widely challenged. Were drug development such a risky proposition, then one would expect that from time to time the fortunes of corporations would vary. On the contrary, since 1980, all the large corporations have done well financially. As Stanley Finkelstein, a physician, and Peter Temin, an economist, both based at the Massachusetts Institute of Technology, point out, “No matter how many times industry analysts warn that a patent expiration is going to make this or that company vanish, it hasn’t happened.30
The emergence of financialization has been fully incorporated by pharmaceutical companies, which has shifted their drug development and marketing strategy. It is now more crucial than ever that therapeutics successfully make it through the regulatory process, which unfortunately has been corrupted.
Key to the industry’s survival is its ability to extend the period during which it has a monopoly on the sale of products, and that translates into strong intellectual property rights, both in the developed world and in the developing countries that represent the emerging sites of growth. With the threat of price controls looming, the other way of expanding revenue is to increase the volume of prescriptions for existing and new drugs. The approach to that goal is to control the knowledge about how and when drugs should be prescribed.31
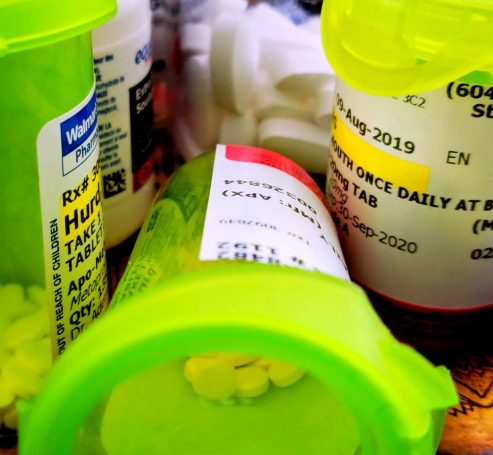 For patients, moving to Medicare for All would provide a direct benefit in this way, unlike any further defense of the ACA. The federal government, as the sole payer for healthcare in the US, would be in a position to negotiate lower drug prices, as is the case in other healthcare systems around the world. Lower drug prices, however, do not check the power and influence of pharmaceutical companies, some of which have essentially become financial institutions rather than research and manufacturing companies, as with the example of Valeant. Medicare for All would not challenge current intellectual property rights that grant monopolies to pharmaceutical companies.
For patients, moving to Medicare for All would provide a direct benefit in this way, unlike any further defense of the ACA. The federal government, as the sole payer for healthcare in the US, would be in a position to negotiate lower drug prices, as is the case in other healthcare systems around the world. Lower drug prices, however, do not check the power and influence of pharmaceutical companies, some of which have essentially become financial institutions rather than research and manufacturing companies, as with the example of Valeant. Medicare for All would not challenge current intellectual property rights that grant monopolies to pharmaceutical companies.
The Communist Party has an opportunity to capitalize on the growing public understanding of the power of the pharmaceutical industry and conceptualize reforms that finally end its continuation as a for-profit industry. Although nationalization and consolidation of the entire industry should consistently be highlighted as the end goal, advocating only for nationalization at this time is not likely to draw significant public support, even from healthcare workers. There are, however, more “reasonable” reforms that the Party can begin demanding and organizing around. First, the Party can demand that the development and approval of any therapeutic that utilizes public funds becomes public property. Subsequent sale of such therapeutics would be at cost. Consider the recent development of COVID vaccinations by private entities using public funds. The pharmaceutical industry is likely to threaten to discontinue research and development of important therapeutics, but that would be the moment to push for nationalization or the expansion of existing public institutions towards therapeutics research and development. Second, the Party can demand that therapeutics production and the regulatory process be divorced entirely from pharmaceutical industry influence. The evaluation and regulation of all therapeutics should be in control of public scientific institutions and be made transparent to the public. From Health Care under the Knife:
To avoid these scenarios [of decreased sale of products] and continue to expand revenue, corporations have evolved from controlling the development of new drugs to controlling the knowledge about those drugs, ensuring that their message is the one that reaches doctors and patients. Pharmaceutical corporations fund almost all pre-market clinical trials, the ones used as the basis for approving a new drug or a new indication for an existing drug. These trials are the foundation of knowledge about a drug and as such their outcome is extremely important. As funders, corporations control all aspects of the trials from their initial design to the way that they are conducted and analyzed, how they are reported to drug regulatory agencies such as the FDA, whether and how they are published, and to a large extent how they are presented to doctors.31
Pharmaceutical industry influence among healthcare workers is well documented. A study of survey results among NPs found that 96% of NPs had regular contact with pharmaceutical representatives, and 48% stated that they were more likely to prescribe a drug that was highlighted during a lunch or dinner event.32 Unfortunately, physicians are not immune to such “soft” influence. One need look no further than the number of physicians that sit on the board of directors of biomedical research and pharmaceutical companies, or physicians in leadership positions at academic medical institutions with ties to these same companies, often as consultants.
The Communist Party can advance real, transformative reforms that would severely curtail the power and influence of the pharmaceutical industry — reforms which can be organized around and draw popular public support.
Unresolved challenges — medical research and publication
In addition to the concerns raised by the influence of the pharmaceutical industry over medical research and the therapeutic regulatory process, there are other related challenges that remain untouched by current healthcare reform proposals. Medicine, like all scientific disciplines, is a perpetually evolving and advancing science. Crucial to this process is the publication of well-designed and peer-reviewed studies that advance our collective knowledge. Despite its central importance, access to medical journals and other publications is severely restricted for those outside academia. Well-respected journals typically charge individuals hundreds of dollars each year, and academic medical institutions pay many thousands of dollars to provide journal access to their healthcare employees. This financial limitation makes it more difficult to keep updated with trends in various medical specialities. It also makes it difficult for the public to access journal articles for themselves. Additionally, there is often strong pressure exerted on healthcare workers, particularly by academic medical institutions, to conduct and publish research. This pressure is quite literally the entire assessment of one’s value as an employee should they be a PhD student or a postdoctoral researcher.
Interestingly, the government of India has shown a potential path forward. A recent “Science, Technology, and Innovation Policy” statement being considered by the government of India proposes,
The Government of India will negotiate with journal publishers for a “one nation, one subscription” policy whereby, in return for one centrally-negotiated payment, all individuals in India will have access to journal articles. This will replace individual institutional journal subscriptions. . . . Full text of final accepted author versions of manuscripts (postprints and optionally preprints) along with supplementary materials, which are the result of public funding or performed in publicly funded institutions, or were performed using infrastructure built with the support of public funds will be deposited, immediately upon acceptance, to an institutional repository or central repository. . . . All data used in and generated from public-funded research will be available to everyone (larger scientific community and public) under FAIR (findable, accessible, interoperable and reusable) terms. Wherever applicable, exceptions will be made on grounds of privacy, national security and Intellectual Property Rights (IPR). Even in such situations, suitably anonymised and/or redacted data will be made available. In all cases, where the data cannot be released to the general public, there will be a mechanism to release it to bonafide/authorised researchers.33
 Such a shift would provide transparency to the general scientific process and democratize access to biomedical knowledge. This need not compromise the necessary protocols to ensure that all scientific literature is of the highest quality, and a concurrent push should be to uniformly institute rigorous standards for all scientific and medical journals. This point is important to consider, as poorly designed studies and/or those that advance wholly pseudoscientific claims (e.g., homeopathy, faith healing and energy therapy, anti-vaccination, traditional Chinese and Ayurvedic medicine), usually rejected by more reputable journals, are published in less rigorous journals that often only demand a direct publication fee. Yet, given the potential “business opportunities” such pseudoscience generates, the possible damage to public health, individual finances, and the underlying trust between the public and the medical profession is immense.
Such a shift would provide transparency to the general scientific process and democratize access to biomedical knowledge. This need not compromise the necessary protocols to ensure that all scientific literature is of the highest quality, and a concurrent push should be to uniformly institute rigorous standards for all scientific and medical journals. This point is important to consider, as poorly designed studies and/or those that advance wholly pseudoscientific claims (e.g., homeopathy, faith healing and energy therapy, anti-vaccination, traditional Chinese and Ayurvedic medicine), usually rejected by more reputable journals, are published in less rigorous journals that often only demand a direct publication fee. Yet, given the potential “business opportunities” such pseudoscience generates, the possible damage to public health, individual finances, and the underlying trust between the public and the medical profession is immense.
Insisting on uniform, rigorous standards of study design, review, and publication also would lessen the influence of charlatans and snake-oil salesmen (and women). Again, given the political economy of healthcare under capitalism, fraudulent claims surrounding diet pills, vitamins/ supplements, CBD/medical cannabis, essential oils, etc. are routinely broadcast and magnified without consequence because they generate profit, despite no evidence of therapeutic benefit and real evidence of harm. Quacks such as Dr. Mehmet Oz, Oprah Winfrey, Gwyneth Paltrow, and the established medical professionals of “complementary and alternative medicine” or “integrative medicine” and their political benefactors in Congress make enormous sums of money while misleading the public and sometimes even delaying life-saving medical care. Capitalist healthcare thrives on quackery, but it is incompatible with the demand for high-quality healthcare under socialism.
The Communist Party can advocate for the democratization of scientific knowledge and improved transparency in medical research. Concurrent with this can be the demand for rigor in the design, execution, review, and publication of scientific studies. Healthcare professionals, in particular, rely upon these studies to inform clinical decision making, and so the production and distribution of scientific knowledge can also be framed as a public good. Furthermore, the Communist Party can gain additional legitimacy by clearly demanding that high-quality healthcare explicitly means that unsubstantiated and demonstrably pseudoscientific claims/products are not compatible with socialized medicine. Medical quackery does real public harm, is tremendously wasteful, and only feeds consumption for the sake of consumption.
Next steps
The historical and present struggle for healthcare reform, reflecting the development of capitalism in its unique social and political environment in the US, has almost entirely focused on insurance. The ACA was devised as a means of ensuring continued revenue for insurance companies, but its abject failure, especially during the COVID pandemic, is now evident for all to see. Medicare for All would bring substantive improvements to the structure of healthcare, but not nearly enough. Unfortunately, the Party Program currently provides no outline of any possible transition or series of reforms that could bridge a Medicare for All system to socialized medicine. Perhaps more importantly, the current Party position on healthcare, largely a reflection of contemporary bourgeois discussions, fails to address corollary challenges that directly impact the material conditions and well-being of healthcare workers. This is unsurprising for either of the bourgeois political parties but is a tremendous, lost opportunity for a revolutionary, Marxist-Leninist party.
The Communist Party can commit itself to expanding and deepening its analysis of the challenges of healthcare in the US by incorporating previously unmentioned issues including medical education, training/working conditions, the undermining of proven and beneficial team-based models of care by non-physician providers, the continued parasitism of the pharmaceutical industry, and the challenges facing medical research and publication. There can also be an attempt to devise a vision of the future transitory steps required to eventually realize socialized medicine in the US, which can be done through establishment of a national healthcare commission or working group. There is a hunger among healthcare workers for a succinct, coherent, and revolutionary challenge to the dominant institutions that manage and oversee the production and distribution of healthcare and its laborers. The Communist Party has an opportunity to rise to the occasion and can provide the lead in that challenge to capitalist power.
Therefore, the Communist Party can commit itself to:
- Establishing a national healthcare commission or working group to research topics of special interest to healthcare, public health, and medical and healthcare professionals
- Demanding greater representation for racial, ethnic, and gender minorities in undergraduate and graduate healthcare programs
- Demanding the full public funding of undergraduate and graduate healthcare programs
- Demanding reforms to the basic structure of medical education
- Demanding increased funding for additional residency spots for physicians, which can be accomplished at existing institutions or at new hospitals and academic medical centers
- Demanding increased funding for preventative healthcare services
- Demanding improved access to high-quality healthcare through the planned construction of hospitals, clinics, and accessory facilities throughout the country
- Demanding increased funding to address failing infrastructure and the poverty of communities’ built environment (i.e., the social determinants of health)
- Demanding the unionization of all healthcare workers
- Demanding limitations to physician work hours and/or increased resident physician salaries to bring about real, meaningful “work-life balance”
- Demanding the primacy of team-based, physician-led, patient-centered healthcare as a human right
- Demanding the categorical abolishment of private health insurance companies
- Demanding the categorical abolishment of private pharmaceutical companies
- Demanding greater transparency and the highest standards of rigor for all scientific studies, including the design, execution, review, and publication of medical research
- Demanding the categorical abolishment of pseudoscientific, unethical, and unsafe practices and products from the healthcare system
- Demanding the categorical elimination of all medical debt
Sources
[1] Luke Savage, “The Coronavirus Has Created Record Support for Medicare for All,” Jacobin.
[2] Efrain Talamantes, et al. “Closing the Gap — Making Medical School Admissions More Equitable,” New England Journal of Medicine.
[3] Association of American Medical Colleges, “Diversity of U.S. Medical Students by Parental Income,” AAMC.
[4] Shin Mei Chan and Jamieson O’Marr, “The Financial Barriers of Applying to Medical School,” KevinMD.com.
[5] David Himmelstein, Steffie Wollhandler, and Howard Waitzkin, Health Care under the Knife: Moving beyond Capitalism for Our Health, chap. 4, 60–61.
[6] Physicians for a National Health Program, “Beyond the Affordable Care Act: A Physicians’ Proposal for Single-Payer Health Care Reform,” PNHP.
[7] Colleen M. Flood and Lorian Hardcastle, “A Two-Tier Health Care System: The New Zealand Story,” SSRN.
[8] Association of American Medical Colleges, “Physician Education Debt and the Cost to Attend Medical School: 2020 Update,” AAMC.
[9] American Association of Colleges of Nursing. “The Numbers behind the Degree: Financing Graduate Nursing Education,” AACN.
[10] American Association of Colleges of Pharmacy Graduating Student Survey: 2018 National Summary Report, AACP.
[11] Steven Novella, “Osteopathic Medicine—What Is It?,” Science-Based Medicine.
[12] Braden MacBeth, “Quackery in Medical School: Chapman Points,” Science-Based Medicine.
[13] Darryl S. Weiman, “Who Pays for Resident Salaries?,” Huffpost.
[14] Association of American Medical Colleges, “Survey of Resident/Fellow Stipends and Benefits Report: 2019–2020,” AAMC.
[15] Benjamin Doolittle, “ACGME Duty Hours Not the Only Big Change in Requirements,” NEJM.
[16] Meghana Karande, et al., “Physician Burnout: The Silent Killer,” GoInvo.
[17] Pamela Wible, “What I’ve learned from 1,513 Doctor Suicides,” Pam Wible MD.
[18] Pamela Hartzband and Jerome Groopman, “Physician Burnout, Interrupted,” NEJM.
[19] American Association of Nurse Practitioners, “Issues at a Glance,”AANP.
[20] Niran Al-Agba and Rebekah Bernard, Patients at Risk: The Rise of the Nurse Practitioner and Physician Assistant in Healthcare, Introduction, xvi–xvii.
[21] Danny R. Hughes, et al., “A Comparison of Diagnostic Imaging Ordering Patterns between Advanced Practice Clinicians and Primary Care Physicians Following Office-Based Evaluation and Management Visits,” JAMA.
[22] Robert H. Lohr, et al., “Comparison of the Quality of Patient Referrals from Physicians, Physician Assistants, and Nurse Practitioners,” Mayo Clinic Proceedings.
[23] Christianne L. Roumie, et al., “Differences in Antibiotic Prescribing among Physicians, Residents, and Nonphysician Clinicians,” JAMA.
[24] M. James Lozada, et al., “Opioid Prescribing by Primary Care Providers: A Cross-Sectional Analysis of Nurse Practitioner, Physician Assistant, and Physician Prescribing Patterns,” Journal of General Internal Medicine.
[25] Primary Care Coalition, “Issue Brief: Collaboration between Physicians and Nurses Works,” PCC.
[26] Physicians For Patients, “So Many Doctors, What Is the Difference?,” PFP.
[27] NewsNation Now, “Families Sound Alarm on Medical Transparency after Deaths of Their Children,” video.
[28] Niran Al-Agba and Rebekah Bernard, Patients at Risk: The Rise of the Nurse Practitioner and Physician Assistant in Healthcare, chap. 4, 72.
[29] Al-Agba and Bernard. Patients at Risk, chap. 1, 11.
[30] Joel Lexchin, Health Care under the Knife: Moving beyond Capitalism for Our Health, chap. 6, 83–85.
[31] Lexchin, Health Care under the Knife, chap. 6, 92.
[32] Elissa C. Ladd, et al., “‘Under the Radar’: Nurse Practitioner Prescribers and Pharmaceutical Industry Promotions,” American Journal of Managed Care.
[33] Department of Science and Technology, Government of India. Draft 5th National Science, Technology, and Innovation Policy for public consultation, DST.
Images: top, Heal America, National Nurses United (Facebook); African American doctor (Pixabay); Health care rally, United Workers (CC BY 2.0); Medical school debt, Jernej Furman (CC BY 2.0); Protect nurses, National Nurses United (Facebook); EKG test, Helge V. Keitel (CC BY 2.0); Medicines, Dennis Sylvester Hurd (CC, Public domain); Medical researcher, NIH Image Gallery (CC, Public domain).


 Join Now
Join Now